7 Things to Know About Mental Health and Addiction
When mental health symptoms and substance use overlap, it’s rarely about “bad choices”—it’s usually about pain, overwhelm, and survival.
It’s encouraging that conversations about mental health have become more open in recent years. The more we talk about anxiety, depression, bipolar disorder, PTSD, ADHD, and other mental illnesses, the more we reduce shame and increase access to support.
However, one aspect of this discussion still gets overlooked too often: the connection between mental health struggles and substance use.
When someone is living with both, the experience can feel confusing, exhausting, and isolating — not only for the person who’s struggling, but also for those who care about them. Still, the connection makes sense once we understand one key truth:
For many people, substance use begins as an attempt to cope.
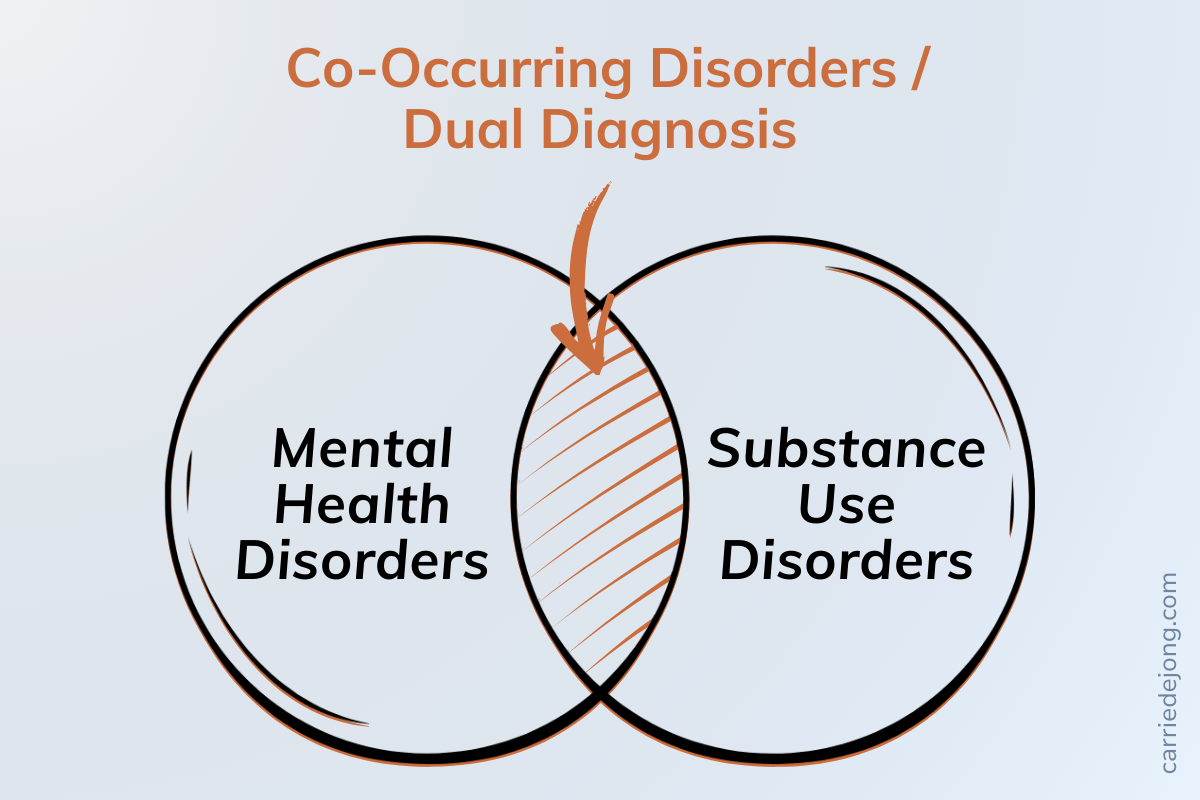
The term co-occurring disorder (also called concurrent disorder or dual diagnosis) describes when a person has both a mental health disorder and a substance use disorder at the same time. The bottom line is simple:
Two issues are present—and both deserve attention.
7 Facts About Co-Occurring Mental Health and Substance Use
1. Co-occurring disorders are common
Many people dealing with anxiety, depression, PTSD, bipolar disorder, or other mental health issues also struggle with alcohol or drug use. For instance, research shows that individuals with anxiety disorders are much more likely to develop alcohol dependence. Panic disorder, in particular, has long been linked to higher risk.
This doesn’t mean everyone with anxiety will develop an addiction, but it does indicate that the connection is more common than most realize.
2. In most cases, the mental health issue develops first
Large studies on co-occurring disorders indicate that for many individuals, mental health symptoms show up first—while substance use develops later. This is important because it helps us see substance use not as “random,” but as something that often arises in response to an already struggling system.
3. Having both tends to make life harder
Mental illness alone can be painful. Addiction alone can be devastating. But when the two occur together, they often intensify each other.
People with co-occurring disorders may experience:
more severe symptoms overall
a longer recovery process
more disruption in relationships, work, and health
greater shame and self-blame
This isn’t because they’re failing. It’s because the nervous system is carrying too much.
4. The two issues often keep each other going
This is sometimes known as mutual maintenance—a cycle in which each problem strengthens the other.
A common example:
Someone drinks to calm anxiety or PTSD symptoms
They feel temporary relief
Then the alcohol wears off
Anxiety rebounds (often worse)
They drink again to get relief
Over time, the brain and body learn that substances are the fastest way to alter an internal state—even though the long-term cost is high.
5. People are less likely to get treatment for both
This is one of the most frustrating realities of co-occurring disorders. Many people never seek treatment at all. And even when they do, they often receive help for only one issue.
Mental health services may not work with someone in active addiction. Addiction treatment may not adequately assess or treat anxiety, depression, trauma symptoms, or ADHD.
When both issues aren’t treated together, people are more likely to relapse—not because they “didn’t try hard enough,” but because the underlying drivers remain unaddressed.
6. Co-occurring disorders can speed up the move into addiction
For many people, substance use begins as a way to find relief. If someone is already dealing with high anxiety, panic, emotional pain, or ongoing emotional dysregulation, substances can seem like a quick, strong fix.
The problem is that the brain adapts quickly, and what starts as a form of coping can turn into dependence faster than people realize.
7. A history of trauma often makes co-occurring disorders more complex
Trauma impacts the nervous system by altering stress responses and affecting how safe (or unsafe) the world feels. When trauma is part of someone’s history, it often raises the risk of mental health issues and substance misuse.
This also explains why relapse happens so frequently: once substances are gone, the original distress returns—sometimes even more intensely.
Before You Go
If you or someone you love is living with both mental health challenges and substance use, it’s important to understand: it’s not a character flaw. Co-occurring disorders often result from a system just trying to survive—trying to manage anxiety, depression, trauma symptoms, shame, or emotional pain as quickly as possible.
With the right support, it’s possible to break this cycle. Healing doesn’t happen through willpower alone—it's achieved through safety, skilled care, and learning new ways to regulate what the mind and body have carried for too long.